Annals of Medical & Surgical Case Reports
Case Report
Mucinous Tubular Spindle Cell Carcinoma of the Kidney: Maybe the Frequently Uncommon is Rendered Common
Nassib F. Abou Heidar1+, M.D.; Jad A. Degheili1+, M.D.; Moustafa A. Moussally1, Jose M. El-Asmar, M.D; Rami W. Nasr1*, M.D.
1Division of Urology, Department of Surgery, American University of Beirut-Medical Center, Raid El-Solh 1107 2020, Beirut, Lebanon
+Both authors contributed equally in this manuscript.
*Corresponding author: Rami W. Nasr, Division of Urology, Department of Surgery, American University of Beirut-Medical Center, Raid El-Solh 1107 2020, Beirut, Lebanon,Tel: 009613388743; Email:rn05@aub.edu.lb
Citation: Nasr RW, Abou Heidar NF, Degheili JA and Moussally MA (2019) Mucinous Tubular Spindle Cell Carcinoma of the Kidney: Maybe the Frequently Uncommon is Rendered Common. Ann Med & Surg Case Rep: AMSCR-1000017.
Received date:22 August, 2019;Accepted date:06 September, 2019;Published date:13 September, 2019
Abstract
Mucinous tubular and spindle cell carcinoma of the kidney is a rare variant of renal cell carcinoma, with a low grade, low malignant potential, and overall favorable prognosis. It is difficult to distinguish from other subtypes of renal cell carcinoma. We are reporting a 72-year-old man with incidental right renal mass after work-up for gross hematuria. Histologically, the tumor consisted of characteristic tubular growth pattern of cuboidal cells, exhibiting eosinophilic cytoplasm, with CK7 positive expression on immunochemical staining. Albeit a rare entity, urologists must identify such rare histological variant of renal cell carcinoma as it carries good prognosis.
Keywords:Mucinous; Renal mass; Spindle cell; Tubular
Abbreviations
MTSCC : Mucinous Tubular and Spindle Cell Carcinoma
RCC : Renal Cell Carcinoma
WHO : World Health Organization
Introduction
There are several subtypes of Renal Cell Carcinoma with a wide array of histological and pathologicalcharacteristics, possessing various clinical behaviors.Mucinous tubular and spindle cell carcinoma (MTSCC) of the kidney represents a rare subtype of RCC which was introduced as a distinct entity by the World Health Organization in 2004[1].MTSCC is comprised of elongated tubules lined by spindle cells that are separated by extracellular mucoid or myxoid stroma. MTSCC has a generally favorable prognosis when complete surgical excision is achieved;thushighlighting the importance of appropriately diagnosing this entitypre-operatively [2].MTSCC is considered as a cytologically low grade neoplasm. Nonetheless, there have been reports of high grade MTSCC as well as reports of sarcomatoid dedifferentiated MTSCC [3,4].
MTSCC has seldom been reported in the literature with less than 100 cases published so far; rendering this tumor a poorly studied entity that poses a great challenge [5].Similar to other renal cell tumors, the majority of MTSCC renal tumors are discovered incidentally; albeit flank pain, abdominal mass, and hematuria are sometimes reported [6].We herein presenta case of72-year-old malewho presented for painless hematuria. Upon investigation, he was found to have MTSCC of the right kidney.
Case Presentation
A 72-year-oldnon-smoker male patientpresented to our urology clinic complaining of multiple episodes of gross painless hematuria over the past 3 months with no other urinary complaints. The patient had a history of benign prostatic hyperplasia, maintained on alpha blockers, without any significant past medical or family history.Routinelaboratory investigations revealed no abnormalities, except for microscopic red blood cells in the urine.An ultrasound of the kidneys and pelvis revealed a new hypoechogenic and suspicious mass, measuring 4 by 3 cm, arising from the upper pole of the right kidney, which was not apparent on a previous ultrasound done three years ago upon evaluation for prostate size and post-void residue. The bladder looked normal with no intramural lesions. Following that, a dedicated image of the renal mass was performed using an enhanced MRI of the abdomen usingGadolinium. A 3.5 by 3 cm clearly marginated lesion was noted at the upper pole of the right kidney arising from the cortex and extending eccentrically, superiorly and posteriorly, corresponding to a RENAL nephrometry score of 6p.The lesion revealed faint mild and progressive pattern of contrast enhancement(Figure 1).As such, the lesion was thus highly suspicious for renal cell carcinoma. After providing all options to the patient including: active surveillance, radio frequency ablation, or surgery;a decision was made to proceed with robotic-assisted laparoscopic right partial nephrectomy.
On gross examination, a 3.5 cm × 3.5 cm × 3.3cm tan-white multinodular mass was seen to be focally disrupting and extruding from the capsule.Histological examination revealed tumor cells with mucoid background. The tumor cells formed small tubular structures, cords and occasional papillae. In addition, theywere cuboidal in shape with a small uniform round nuclei. In some areas, the cuboidal cells mergedwith spindle cell areas forming a similar bland nuclei. There were few mitotic figures andno significant cytologic atypia(Figure 2). According to these findings, a diagnosis of mucinous, tubular, and spindle cell renal cell carcinoma was made.
The post-operative course was smooth and patient was discharged home on post op day 3. One year after surgery, no evidence of disease recurrence was noted.
Discussion
Mucinous tubular and spindle cell carcinoma (MTSCC) is a low grade pleomorphic renal epithelial neoplasm that has an indolent clinical behavior. MTSCC has a female predilection with a female-to-male ratio of 4:1 andan age range from 13 to 82 years[2,6].Although initially thought to originate from collecting duct epithelium or cells of the loop of Henle, recent evidence has speculated that this tumor most likely originates from proximal nephronsrelating it closely to papillary RCC [7,8].This was concluded upon the tumor’s expression of an epithelial marker, alpha-methylacyl-Coenzyme A racemase (AMCAR), which is seen in proximal convoluted cells [9].
On histological examination, MTSCC is composed of tightly packed, ovoid tubules that are elongated with a pale basophilic mucin and myxoid stroma separating the tubular cells.In MTSCC, the cells are cuboidal with a transparent cytoplasm and a low-to-medium sized nucleoli. Furthermore, mitotic figures are rarely seen [5,7]. MTSCC has several variants which include mucin poor MTSCC and MTSCC with neuroendocrine differentiation. Recent case reports have described aggressive types of MTSCC presenting with distant metastasis and associated with fatal outcomes[3,4].
Due to histological similarities, MTSCC is often confused with other subtypes of RCC such as sarcomatoid RCC, papillary RCC, and collecting duct carcinoma (CDC). However, MTSCC’s favorable prognosisjustifies the need for suitable distinction between MTSCC and other subtypes of RCC [2,3].Alcian blue acidic mucin is the most reliable method of segregation2, 6, whereas immunohistochemistry offers little aid in differentiating between MTSCC and the papillary type of RCC since both have an almost similar immunohistochemical staining profiles.1 Morphologic features need to be combined with immunohistochemistry, and spindle cell is an important diagnostic clue for MTSCC. On the other hand, MTSCC lacks the typical genetic alterations seen in papillary RCC such as an absent Y-chromosome. In contrast, MTSCC has been associated with other chromosomal losses such as chromosomes 1,4,18, 22 and others 2.
On imaging, MTSCC can be distinguished from clear cell RCC by the decreased enhancement of the cortex during the corticomedullary phase. However, the enhancement characteristics of MTSCC are similar to those of papillary RCC making the distinction unreliable [1,11,12]. The significance of a renal biopsy in diagnosing MTSCC is still debatable due to the paucity of data on this topic[1], which necessitates surgical resection due to the risk of papillary RCC.
There are still no established guidelines pertaining to the management of MTSCC; yet based on the few case reports available in literature, surgical excision seems to be the adequate management for localized disease. In cases of small renal masses, MTSCC cannot be distinguished from other subtypes; hence ablative therapy (cryotherapy, radiofrequency ablation, etc.) represents an option in patients with multiple comorbidities due to their indolent behavior. Moreover, in elderly patients who are poor surgical candidates, active surveillance can be sought of an option [13].
On the other hand, the management of metastatic MTSCC is still debatable with some case reports illustrating the benefits of sunitinib, a tyrosine kinase inhibitor, in reducing tumor burden and possible improvement insurvival [3,6,13-15].In contrast, a recent case report revealed no benefits of systemic treatment with Pazopanib in treating an advanced case of MTSCC [3].In conclusion, further investigation is warranted in order to set the guidelines for the treatment of metastatic MTSCC.
Conclusion
Renal masses remain a diagnostic dilemma among clinicians, with little available resources for discernment of the main pathology and their respective malignant potential. This is a case of a rare renal carcinoma subtype, exhibiting a low malignant potential and favorable outcome. Surgical resection remains necessary in these scenarios when radiological features lag behind pathological confirmation. Adherence to treatment guidelines of renal masses, which is still evolving, should be applied, despite the ongoing changes in renal carcinoma classifications.
Consent:Written Informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Authors’ Contributions: JD and RN performed surgery for the patient. The manuscript was initially written by JD, NAH, and MM. Literature review was performed by MM, NAH and JE. CK provided the pathological/ histological images and their respective descriptions. JD, NAH, and RN edited the manuscript.All authors have approved the final version of the manuscript prior to submission.
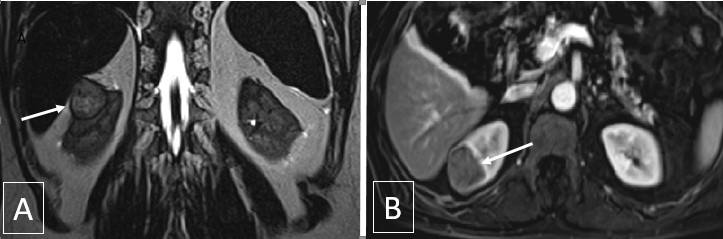
Figure 1: A) Magnetic resonance image (MRI) T2-weighted revealing a 3.5cm right kidney upper pole mass arising from the cortex, R.E.N.A.L. nephrometry score: 6p. B) T1 contrast imaging after gadolinium injection; the mass portrays a delayed pattern of contrast enhancement.
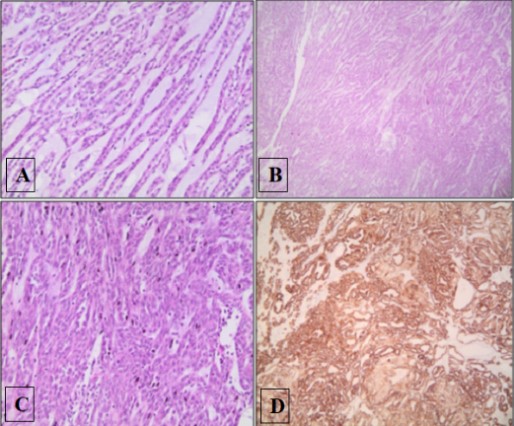
Figure 2:A) Image showing an area of low cuboidal cells with eosinophilic cytoplasm, arranged in tubules, with low mitotic figures and no significant cytological atypia (hematoxylin-eosin stain; original magnification x20). B) Image showing the characteristic tubular growth pattern in mucinous spindle cell carcinoma with a myxoid/mucoid background (hematoxylin-eosin stain; original magnification x4). C) Image showing an area of anastomosing spindle cells that lacks the tubular growth pattern (hematoxylin-eosin stain; original magnification x20). D) CK7 immunohistochemistry staining positive in mucinous tubular and spindle cell carcinoma (original magnification x4).
Citation: Nasr RW, Abou Heidar NF, Degheili JA and Moussally MA (2019) Mucinous Tubular Spindle Cell Carcinoma of the Kidney: Maybe the Frequently Uncommon is Rendered Common. Ann Med & Surg Case Rep: AMSCR-1000017.