Annals of Medical & Surgical Case Reports
Myaesthenia Gravis with Congenital Dermoid Ambylopia
Anubhav Chauhan1*, Poonam Samyal2 and Kulbhushan Prakash Chaudhary3
1Department of Ophthalmology, Dr Yashwant Singh Parmar Government Medical College, Nahan, Himachal Pradesh, India
2Student-Obstetrics and Gynaecology, Kamla Nehru Hospital, Himachal Pradesh, India
3Department of Ophthalmology, Indira Gandhi Medical College, Himachal Pradesh, India
*Corresponding author: Anubhav Chauhan, Department of Ophthalmology, Dr Yashwant Singh Parmar Government Medical College, Nahan, District Sirmour, Himachal Pradesh, India, Tel: +919816991482.
Citation: Chauhan A, Samyal P, Chaudhary KP (2019) Myaesthenia Gravis with Congenital Dermoid Ambylopia. Ann Med & Surg Case Rep: AMSCR: 100004
Received Date: 08 April, 2019; Accepted Date: 16 April, 2019; Published Date: 26 April, 2019
Case Report
A 52-year-old female patient (Figure 1) presented to the ophthalmology department with a history of itching bilateral eyes off and on for the past few months. She was a known case of myaesthenia gravis (MG) and was on tablet pyridostigmine (Acetycholinesterase inhibitor-60 mg daily dose) for the past three years from some medical specialist. There was no other ocular complaint nor there was any history of previous ophthalmic consultation. There was no other significant medical, surgical, family, traumatic or other drug intake history. The positive findings on her ocular examination (Figure 2a and 2b) was visual acuity of 6/6 in the left eye and 2/60 in the right eye with no improvement on pinhole. There was a high myopic astigmatism, divergent squint and a limbal dermoid in the right eye plus bilateral mild ptosis but absence of diplopia. Fundus examination of the right eye revealed large vertically oblong optic disc with temporal crescent and the patient had an eccentric fixation. Fundus examination of the left eye was normal. Slit lamp examination revealed allergic conjuctivitis in both the eyes. The pupillary reactions, ocular movements, colour vision, intraocular pressure were normal bilaterally.
On further questioning, the patient stated that the mass (limbal dermoid) in the right eye was present since childhood. There is no dermoid/growth in the other eye. She was also on treatment for allergic rhinitis. There was no other significant finding on general physical and systemic examination ruling out an associated Goldenhar syndrome. The ambylopia in the right eye could be a consequence of the dermoid. A diagnosis of myaesthenia gravis with bilateral allergic conjuctivitis plus ambylopia and limbal dermoid right eye was made.
We believe that the dermoid was the most probable cause for ambylopia because:
a. The ptosis had developed in adulthood when the patient developed myaesthenia gravis and not during the plastic period (ambylogenic age) i.e before 6 years of age.So it cannot be the cause of ambylopia.
b. Secondly, any mass or growth in the corneal and limbal area like pterygium, dermoid, ocular surface squamous neoplasis etc can lead to significant astigmatism. So, as this growth was present since birth and even a small degree of astigmatism i.e upto 1.5 diopters can be ambylogenic.
The patient was started on topical olopatadine for allergic conjuctivitis and was advised follow up. The presence of limbal dermoid in MG could be a coincidental finding or may have an association. To the best of our knowledge and after an intensive internet search, this is probably the first reported case of limbal dermiod with MG.
Discussion
Acquired MG is a relatively uncommon disorder, with prevalence rates that have increased to about 20 per 100,000 in the US population. In about 10% of myasthenia gravis patients, symptoms are limited to extraocular muscles. Below 40 years of age, female: male ratio is about 3: 1; however, between 40 and 50 years, it is roughly equal. Over 50 years, it occurs more commonly in males. Subtypes of MG are broadly classified as follows:
(1) Early-onset MG: age at onset <50 years. Thymic hyperplasia, usually females
(2) Late-onset MG: age at onset >50 years. Thymic atrophy, mainly males
(3) Thymoma associated MG (10%-15%)
(4) MG with anti-MUSK (muscle-specific tyrosine kinase) antibodies
(5) Ocular MG: symptoms only affecting extraocular muscles
(6) MG with no detectable AChR (acetylcholine receptors) and MuSK antibodies [1].
MG is characterized by a variable weakness of skeletal muscles, which improves on resting. Bulbar, limb, respiratory and extraocular muscles (levator and orbicularis oculi muscles) are commonly involved. Ptosis and diplopia are common ocular features. Lid fatigability test and Cogan’s lid twitch sign can be seen in ocular MG. The most commonly affected extraocular muscles is the medial rectus followed by the superior rectus. Other tests for MG include sleep test, ice test, Edrophonium test, AChR?antibodies titers, electrophysiologic testing, Computerized tomography (CT) of the chest and thyroid function test [2].
Treatment for MG includes anti-acetylcholinesterase drugs like pyridostigmine, immunomodulatory therapies (intravenous immunoglobulin and plasma exchange), and immunosuppressant medications (steroids, azathioprine, cyclosporine, and methotrexate), thymectomy, eculizumab and rituximab. Drugs under trial include rozanolixizumab, efgartigimod and monarsen [3].
Limbal dermoid is also a part of Goldenhar syndrome. This syndrome is also known as oculo-auriculo-vertebral syndrome. For diagnosis to be confirmed, the subject should at least have microtia and preauricular, or auricular abnormalities [4].
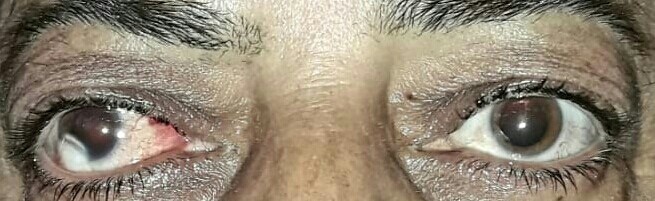
Figure 1

Figure 2a: (right eye)
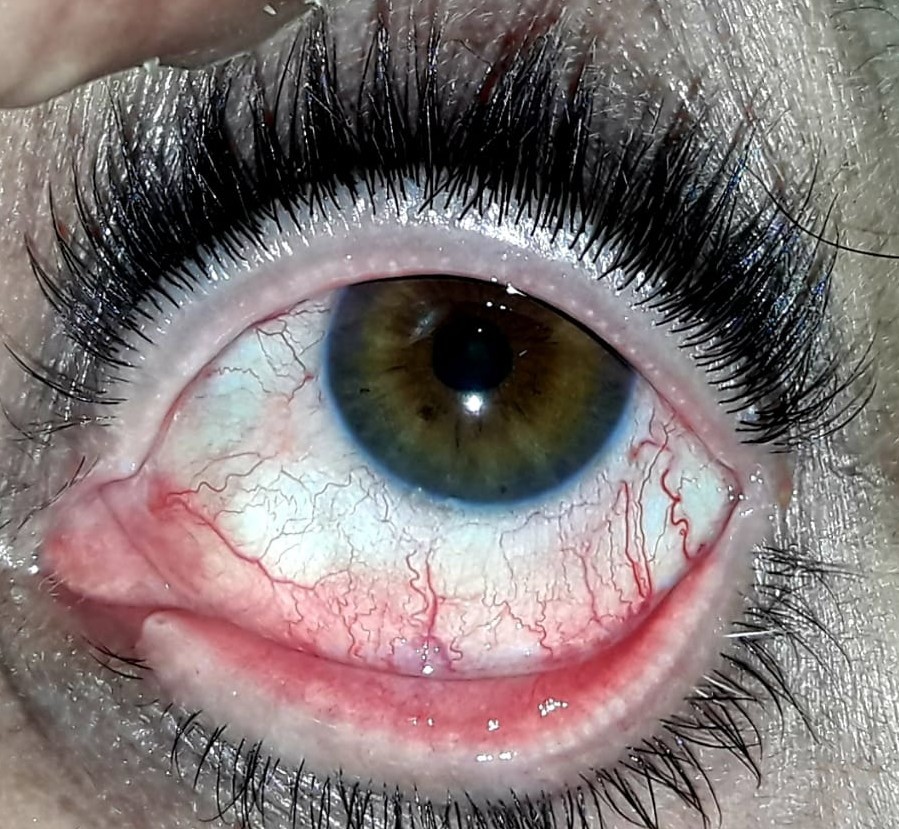
Figure 2b: (left eye)
Citation: Chauhan A, Samyal P, Chaudhary KP (2019) Myaesthenia Gravis with Congenital Dermoid Ambylopia. Ann Med & Surg Case Rep: AMSCR: 100004